|
It can be diagnosed with the aid of echocardiography, axial computed tomography, magnetic resonance imaging, contrast esophagogram and bronchoscopy. It should be thought of double aortic arch in patients with dysphasia, stridor, cough, dyspnea, and upper respiratory tract infections. The first description of this disease were apparently done by Hommel, in 1737, and the first surgical correction was performed by Gross, in 1945. It is known that the double aortic arch is the most common form of vascular ring and can be defined as a congenital anomaly in which the aortic arch and its branches surround the trachea and the esophagus completely or incompletely possibly causing compression of these structures. There was also a perimembranous VSD of about 7 mm. 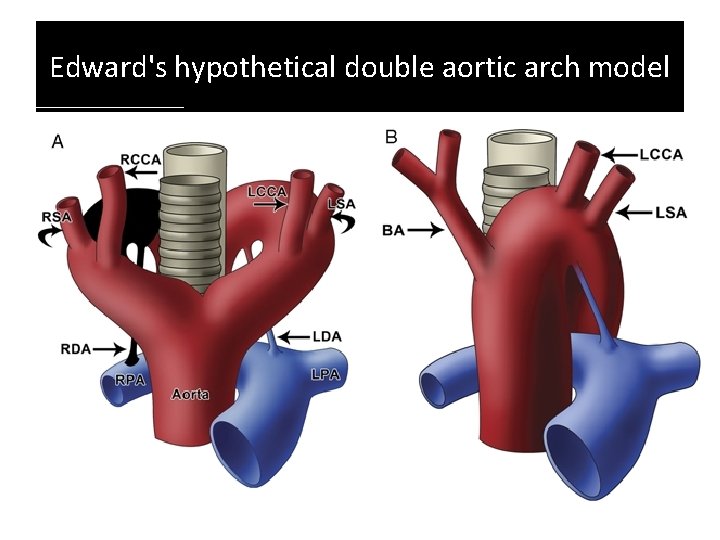
The second arch is smaller (diameter of 4.9 mm), continued to the left as patent ductus arteriosus (average size of 3.7 mm) providing blood supply to the right and left confluent pulmonary arteries ( Figure 1). The dominant arch is positioned to the right with a diameter of 6.7 mm. Double aortic arch without typical vascular ring formation. Descendent aorta positioned to the right of midline. No typical image of pulmonary valve or trunk suggesting pulmonary atresia. Left aortic arch originating the left common subclavian and carotid arteries, interrupted right after the emergence of the patent ductus arteriosus which have a diameter of 2.2 mm. Right aortic arch in continuity with the descendent aorta originating the right common subclavian and carotid arteries. Confluent pulmonary arteries (diameter: trunk 4.7 mm/3.9 mm right pulmonary artery/3.6 mm left pulmonary artery), absent right ventriculoarterial connection. 
Presence of wide perimembranous ventricular septal defect (VSD), with a bidirectional flow without significant gradient on Doppler. Normal venoatrial and atrioventricular connections. Present and symmetrical peripheral pulses.Įnlarged cardiac area mainly due to right atrial enlargement. Presence of systolic murmur 4+/6+ predominantly at the lower left sternal border. Upon physical examination presented at a regular general condition, eupneic in use of an oxygen mask with saturation around 97%. Preterm newborn at the 35 th week, second day of life, 2.7 kg, male, referred to our service after presenting respiratory distress associated with cyanosis. TGA = Transposition of the great arteries
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
